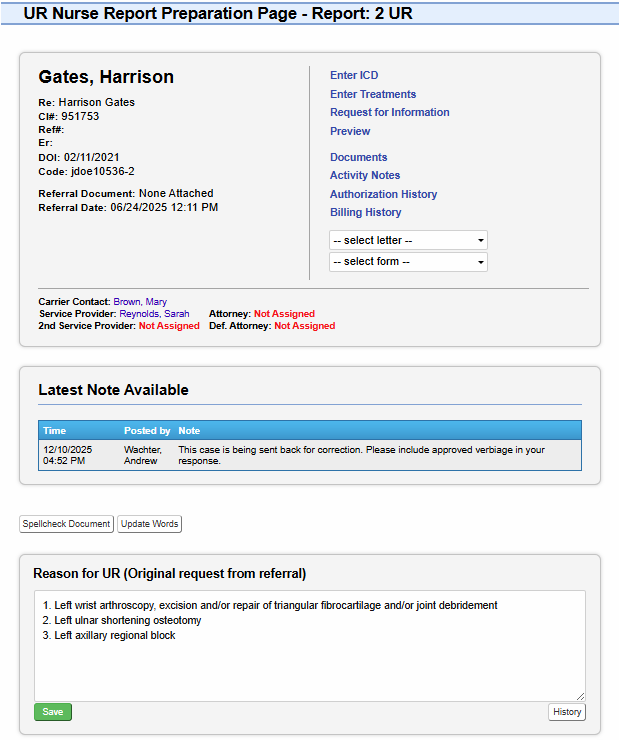
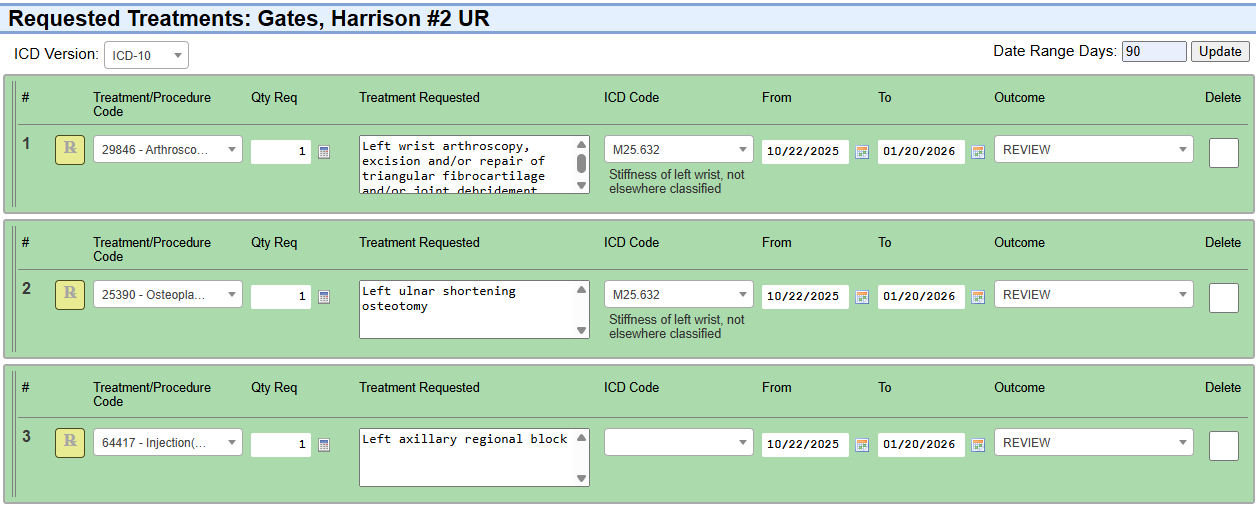
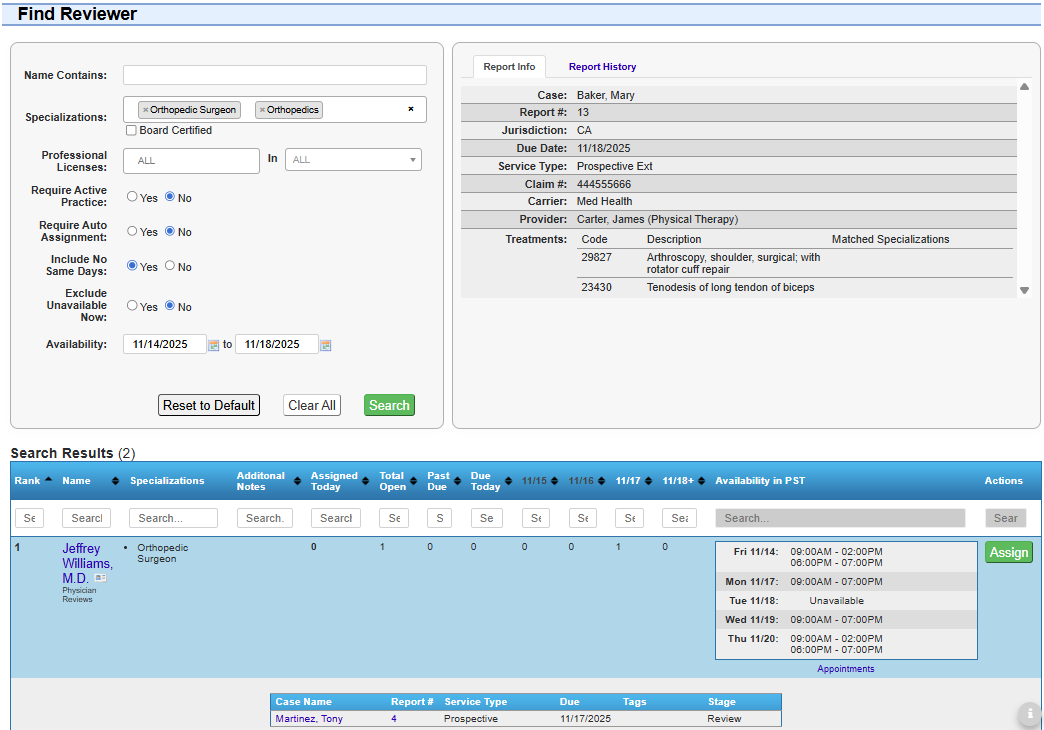
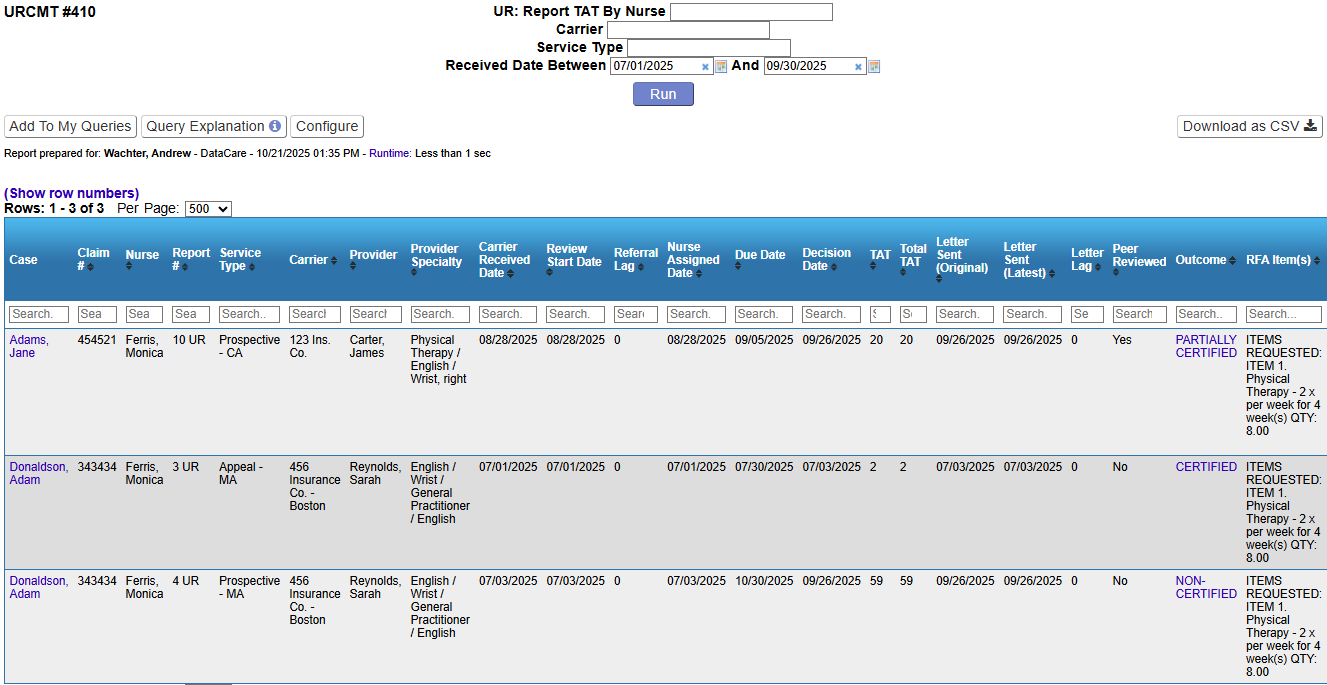
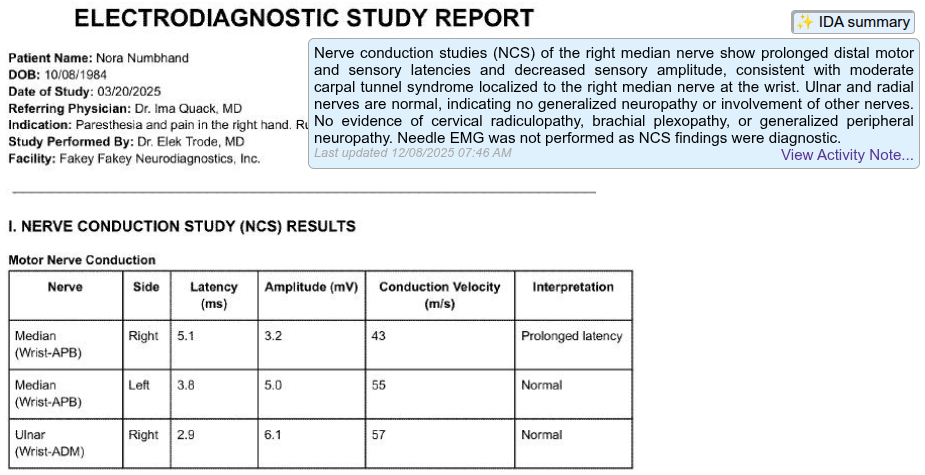
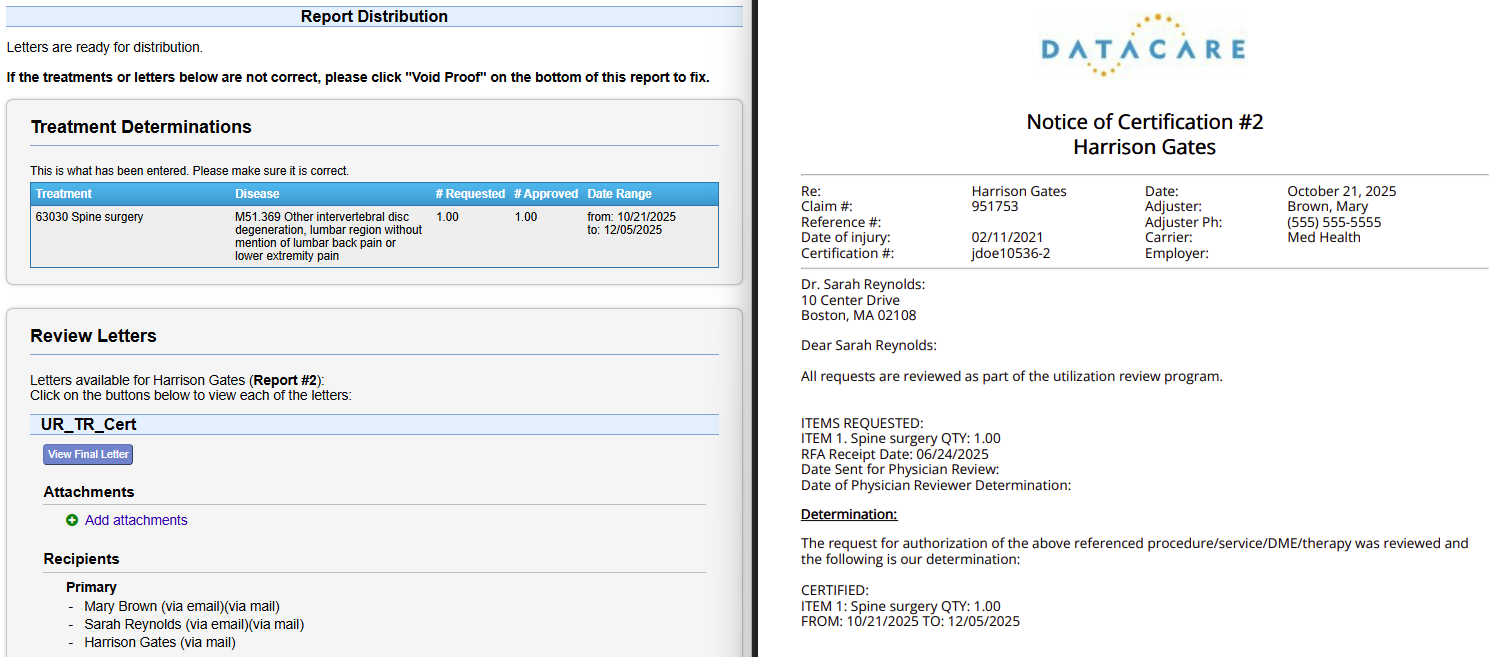
Structured, Configurable Utilization Review — Built for Speed and Compliance
Bring intake, reviewer assignment, determinations, letters, reporting, and compliance into one workflow — reducing administrative work while improving visibility and control.
Built for workers’ compensation, managed care, peer review, and other regulated medical review teams.
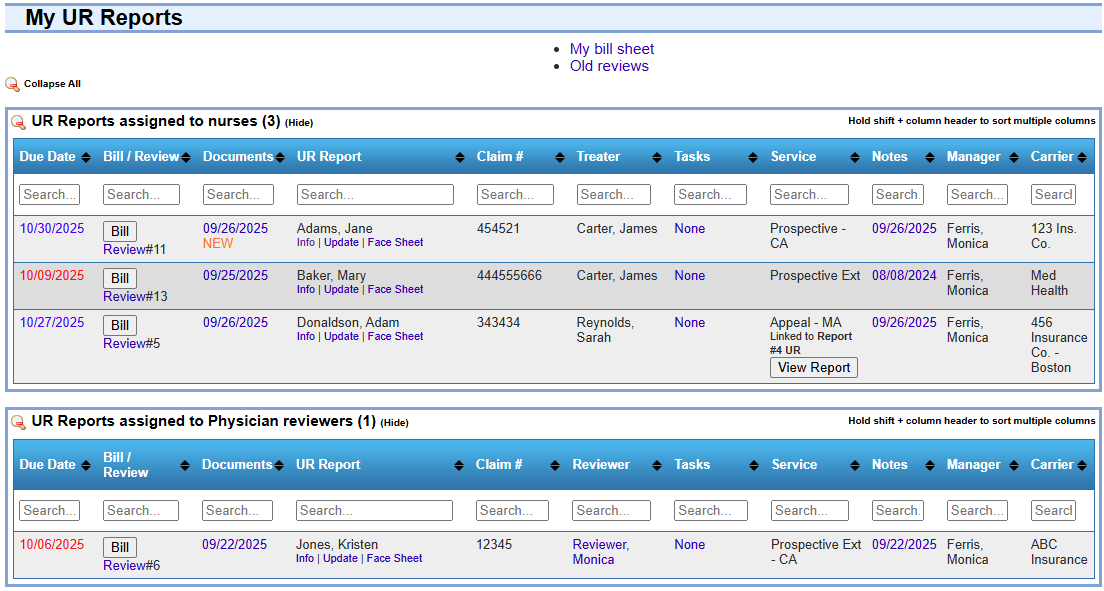

Why UR Teams Outgrow Generic Systems
Proof: Our clients report saving 1-2 hours per UR nurse/physician per day, and some departments report doubling throughput.*
*Time savings are self-reported by customers based on typical case volumes and workflows; results vary.
Structured, Configurable Utilization Review
Built for Real Utilization Review Teams
Everything you need, one login.
Core Features and Benefits
Proven to Improve Workflow Fit, Visibility, and Performance
“DataCare really understands the case management and utilization review ecosystem. Their platform is robust and stable, a must-have in a systems provider. Our focus at Ascential Partners is to promote the right treatment so our patients get back to their lives using the most expedient, cost-effective, and solution-minded way. DataCare is an important partner, helping us with our mission.”
Michele Settel, President of Ascential Care Partners

“The entire team we worked with made every effort to understand our requirements and fulfill them as best as possible. They were open to listening to our users and adapt the Ahshay platform to their needs, this is quite unlike most vendors who are rigid and unwilling to even consider that client requirements may benefit their products. The team on our project was very patient with our end users, who are non-technical.”
Anant Joshi, Information Systems Director at Charter Management